Expand Your Reach
Increase your cyclotron’s production of critical isotopes that are essential to the future of patient care for important disease states within Oncology and Cardiology with ARTMS technology.
Learn How
Innovative Isotopes Have Brought New Hope to Patients
ARTMS has worked with drug innovators and distributors to make sure key isotopes like Ga-68 will be available on demand to the populations that need them most. ARTMS’ ability to empower local cyclotrons to produce large volumes of isotope will ensure that patients will get the right study at the right time.




A QUANTM Leap Forward for Isotope Production
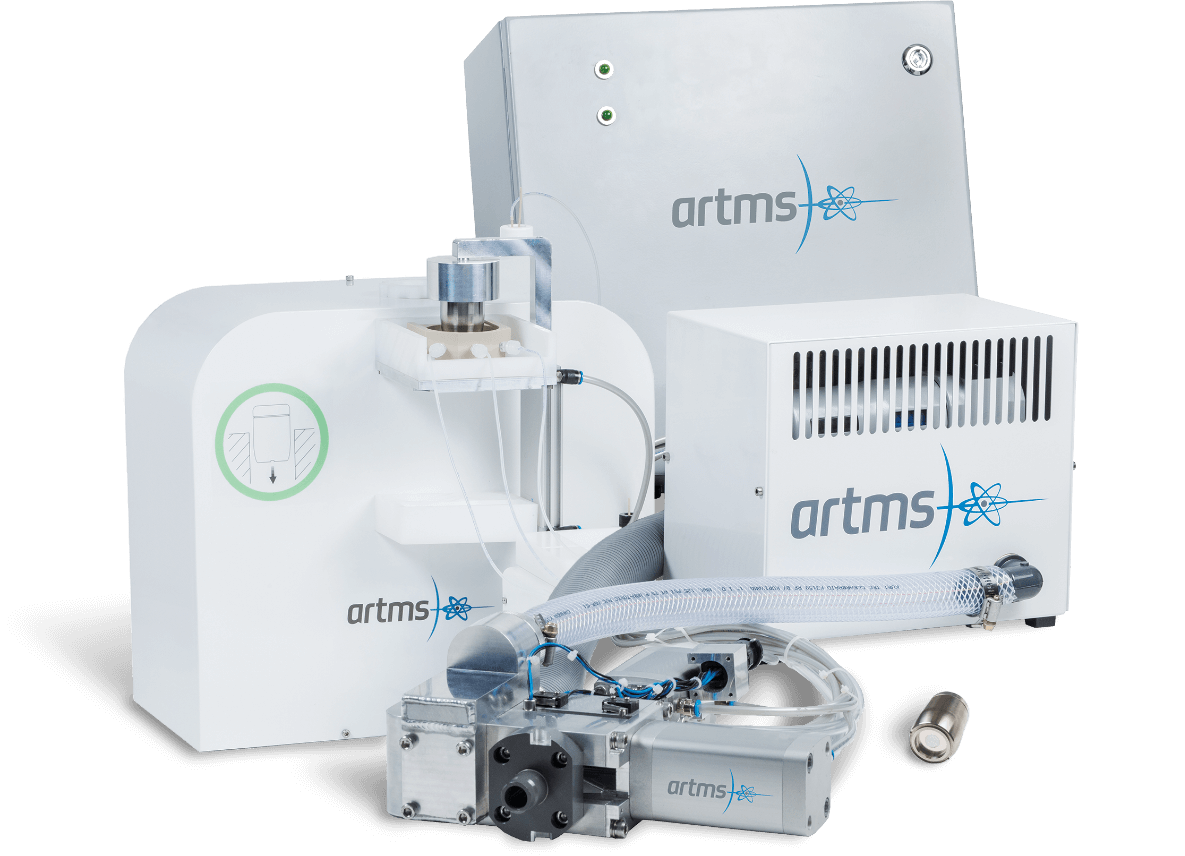
ARTMS produces and supplies QUANTM targets that when paired with the QUANTM Irradiation System (QIS™) and a medical cyclotron allow for production of some of the most impactful nuclear medicine products developed over the past decade. ARTMS technology will significantly decrease the market’s reliance on generator and centrally produced isotopes. This, along with the increase in potential volume, has created a shift in how isotopes are secured.
Discover QUANTM TargetsWhy Build, When You Can Simply Upgrade?
ARTMS technology can be installed on new and currently installed cyclotrons with little to no interruptions of day to day operations. ARTMS is compatible with the most commonly installed cyclotrons globally and does not require any major construction or site modifications.
Adopt The QIS™ Ecosystem

ARTMS (Alternative Radioisotope Technologies for Medical Science) was created to enhance human health through innovation and leadership in medical isotope production. ARTMS is changing the Nuclear Medicine supply chain status quo.


